Shoulder Surgery Risks and Complications in Florida
Key Takeaways
- Shoulder surgery risks and complications are real — but most are rare when the right specialist performs your procedure.
- Infection, stiffness, nerve injury, and implant issues are the complications patients ask about most. All are manageable with proper surgical technique and follow-up.
- Your individual risk profile — age, health history, tear severity — matters more than surgery type alone.
- Non-surgical options exist for many shoulder conditions. A second opinion before committing to surgery is always appropriate.
- Fellowship-trained surgeons with high procedural volume consistently report lower complication rates than general orthopedic providers.
If you’re dealing with persistent shoulder pain — a torn rotator cuff, chronic instability, or a condition that hasn’t responded to conservative care — shoulder surgery has probably come up. And with it, the questions that keep patients up at night: What could go wrong? How bad is the recovery? Am I making the right decision?
Those questions deserve straight answers, not reassurance for its own sake. Shoulder surgery risks and complications are a legitimate part of any informed surgical decision. Understanding them clearly — what they are, how often they occur, and what reduces them — is the foundation of a confident choice.
At Florida Sports Injury & Orthopedic Institute in Clermont, FL, Dr. Amit Varma and the FSI team have this conversation with patients every day. This guide reflects that clinical experience.
What Are the Real Risks of Shoulder Surgery?
Every surgical procedure carries baseline risk. For shoulder surgery specifically, risks fall into two categories: general surgical risks that apply to any procedure, and shoulder-specific complications tied to the anatomy, procedure type, and your health profile.
General surgical risks include anesthesia reactions, blood clots (deep vein thrombosis), wound infection, and bleeding. These are well-understood, screened for in pre-operative evaluation, and managed through standard surgical protocols.
Shoulder-specific risks center on the complexity of the joint itself — a highly mobile structure dependent on a precise balance of tendons, nerves, muscles, and bone. Disrupting that balance, even temporarily through surgery, carries defined risk that a skilled surgeon actively works to minimize.
The American Academy of Orthopaedic Surgeons (AAOS) notes that serious complications from shoulder surgery are uncommon — but they are not zero. Transparency about that is the starting point for a trustworthy clinical relationship.
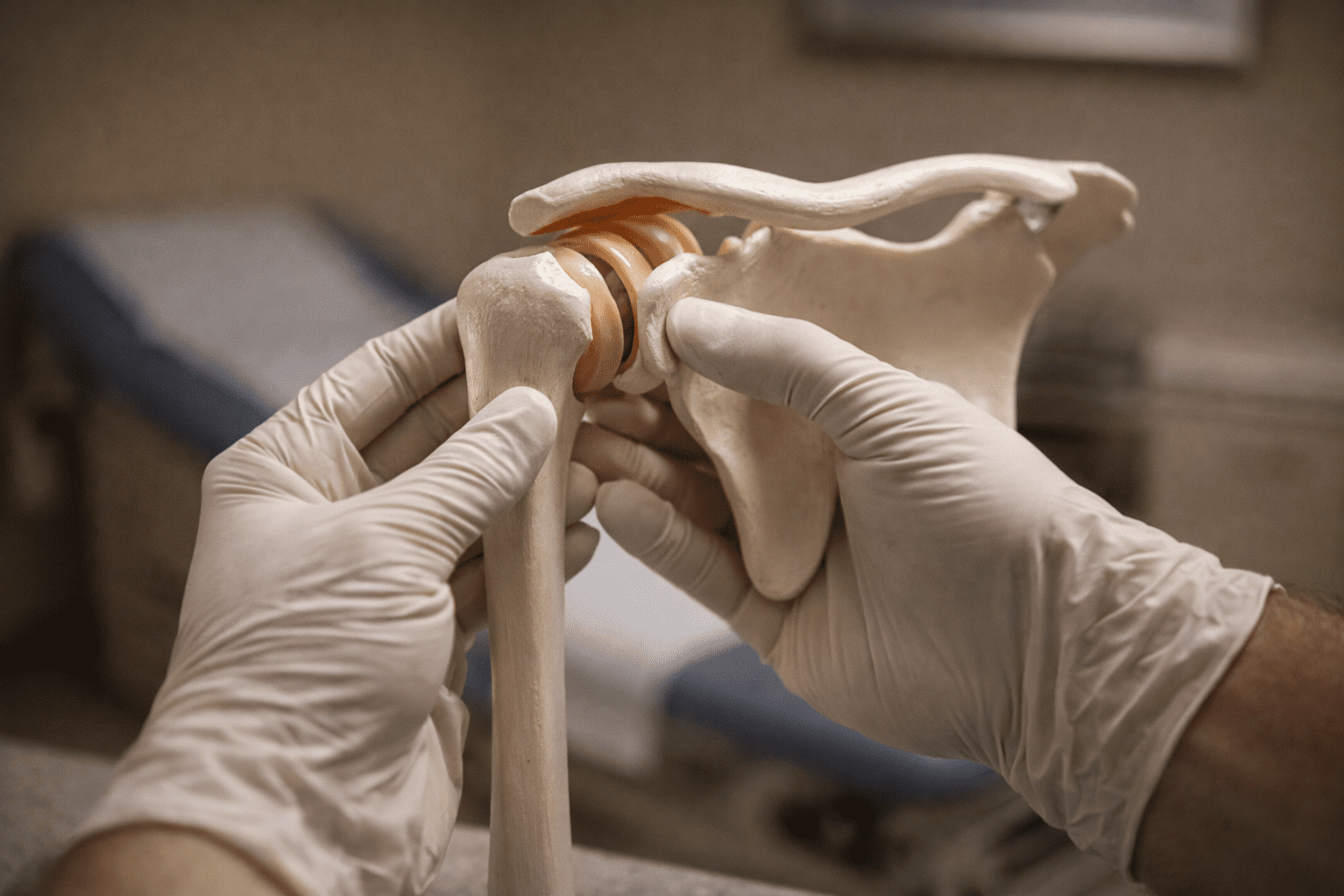
The Most Common Shoulder Surgery Complications
The following are the complications patients ask about most — and what the clinical evidence shows about their actual frequency.
Infection
Post-operative infection rates for shoulder surgery range from 0.5% to 1.9%, with open procedures carrying slightly higher risk than arthroscopic techniques. Propionibacterium acnes (now reclassified as Cutibacterium acnes) is a bacterium naturally present on shoulder skin that accounts for a disproportionate share of shoulder-specific infections — a fact that experienced shoulder surgeons screen and prepare for proactively.
Nerve Injury
The axillary nerve and brachial plexus run in close proximity to the shoulder joint. Temporary nerve irritation occurs in a small percentage of cases and typically resolves within weeks to months. Permanent nerve damage is rare in the hands of a fellowship-trained specialist but carries serious functional consequences when it does occur. Research published in the National Institutes of Health (NIH) documents axillary nerve injury rates under 1% in experienced centers.
Stiffness and Frozen Shoulder
Post-operative stiffness is one of the more commonly encountered shoulder surgery complications — particularly after rotator cuff repair. Adhesive capsulitis (frozen shoulder) can develop when immobilization is prolonged or physical therapy is delayed. Structured early rehabilitation significantly reduces this risk. At FSI, every surgical patient receives a personalized physical therapy protocol beginning in the immediate post-operative phase.
Implant Failure or Loosening
For shoulder replacement procedures, implant loosening is the primary long-term complication. Glenoid component loosening occurs in roughly 5–10% of anatomic total shoulder replacements over 10 years. Reverse shoulder replacements — increasingly used for rotator cuff arthropathy — show different failure patterns, with notching and instability as primary concerns. Surgeon volume and implant selection directly affect these outcomes.
Blood Clots
Deep vein thrombosis (DVT) and pulmonary embolism are rare after shoulder surgery compared to lower extremity procedures but remain a documented risk, particularly in patients with clotting history, obesity, or limited post-operative mobility. Standard prophylaxis protocols reduce this risk substantially.
Rotator Cuff Re-Tear
Re-tear after rotator cuff repair occurs in 15–25% of cases, with larger tears carrying higher rates. Critically, not every re-tear causes pain or limits function — but some require revision surgery. Compliance with rehabilitation, appropriate sling use, and activity restrictions in the first 12 weeks are the primary factors within a patient’s control.
Who Faces the Highest Risk?
Risk is not uniform. Several patient factors consistently correlate with higher shoulder surgery complication rates across peer-reviewed literature:
- Age over 65 — slower tissue healing, higher anesthesia sensitivity
- Diabetes — impaired healing and elevated infection risk
- Smoking — significantly worsens rotator cuff healing outcomes and increases infection rates
- Obesity (BMI >35) — deeper tissue planes, increased surgical complexity
- Large or massive rotator cuff tears — lower biological healing potential, higher re-tear rates
- Prior shoulder surgery — scar tissue, altered anatomy, reduced tissue quality
- Steroid use — chronic corticosteroid use impairs tissue integrity
Knowing your risk profile before surgery allows the care team to modify technique, timing, and post-operative management to account for these factors. An honest pre-operative discussion with your surgeon about your individual risk is non-negotiable.
How Surgeons Reduce Shoulder Surgery Risks
The single greatest modifiable variable in shoulder surgery outcomes is surgeon experience and technique. Shoulder surgery risks and complications are not fixed — they are directly shaped by who performs the procedure and how.
Dr. Amit Varma at the Varma Shoulder Institute is double-board-certified and double-sports fellowship trained, with subspecialty focus in shoulder reconstruction, arthroscopy, and complex revision cases. Subspecialty training means higher procedural volume, deeper anatomical familiarity, and pattern recognition developed across thousands of shoulder cases — all of which translate to measurably better outcomes.
What to ask your surgeon before agreeing to shoulder surgery:
How many of this specific procedure do you perform per year? What is your personal complication rate for this operation? What does your post-operative protocol include, and will I have access to physical therapy through your practice? These are reasonable questions. A qualified surgeon welcomes them.
Other evidence-based risk-reduction strategies used at FSI include:
- Pre-operative skin decolonization protocols targeting C. acnes
- Arthroscopic technique over open surgery wherever clinically appropriate
- Biologic augmentation (PRP, REGENETEN bioinductive scaffold) for high-risk rotator cuff repairs
- Structured, phase-based physical therapy starting in week one post-op
- Active smoking cessation support required before elective shoulder surgery
FSI vs. General Orthopedic Providers: What Matters Most
| Factor | Florida Sports Injury & Orthopedic Institute (FSI) | General Orthopedic Practice |
|---|---|---|
| Surgeon Training | ✔ Double-sports fellowship trained, shoulder subspecialist | ✘ General orthopedic training; may not subspecialize in shoulder |
| Shoulder Case Volume | ✔ High-volume shoulder center with advanced arthroscopic capability | ✘ Variable; shoulder cases may be a fraction of caseload |
| Non-Surgical Options | ✔ PRP, stem cell, targeted injection therapy, structured PT on-site | ✘ Often limited; may refer out for non-surgical management |
| Infection Risk Protocols | ✔ Pre-op C. acnes decolonization, arthroscopic-first approach | ✘ Standard protocols only; may not address shoulder-specific pathogens |
| Biologic Augmentation | ✔ REGENETEN, PRP for rotator cuff repair when indicated | ✘ Often unavailable; not all surgeons are trained in biologics integration |
| In-House Rehabilitation | ✔ Coordinated PT, phase-based protocol, same-practice team | ✘ External referral; care coordination gaps more common |
| Walk-In / Urgent Access | ✔ Walk-in clinic available; same-day evaluation for acute injuries | ✘ Appointment scheduling only; ER for acute situations common |
Surgical vs. Non-Surgical: Weighing Your Options
Surgery is not always the first or only answer. For many shoulder conditions, structured non-surgical treatment produces outcomes that match — or in some populations exceed — surgical results. This is particularly true for:
- Partial-thickness rotator cuff tears in patients over 65
- Mild-to-moderate shoulder impingement
- Degenerative rotator cuff changes without acute functional loss
- First-time anterior shoulder dislocations in older, lower-demand patients
At FSI, Dr. Aalok Shah and Dr. William Athans — both non-operative sports medicine physicians — conduct thorough evaluations to determine whether non-surgical treatment including physical therapy, corticosteroid injection, PRP, or targeted activity modification can resolve your problem before surgery becomes necessary.
The Harvard Health Publishing guidance on shoulder conditions confirms that shared decision-making — where patients understand both surgical and non-surgical pathways — produces better long-term satisfaction and adherence to care plans. Surgery entered into without understanding the alternatives tends to produce worse patient experience outcomes, independent of the clinical result.
📽 Educational Resource — Shoulder Surgery: What to Expect
Video summary: This educational video covers what to expect during and after shoulder surgery — including the procedure itself, sling requirements, activity restrictions, and the general phases of physical therapy recovery. Provided for patient education purposes only.
What Recovery Actually Looks Like
Recovery timelines vary significantly by procedure. Setting accurate expectations before surgery reduces anxiety and improves adherence to rehabilitation — both of which directly influence outcomes.
Arthroscopic Shoulder Surgery (Labrum Repair, Impingement)
Most patients return to desk work within 1–2 weeks. Sling use typically extends 4–6 weeks. Full return to sport or physical labor generally requires 4–6 months, depending on the specific repair performed.
Rotator Cuff Repair
The tendon-to-bone healing process requires 10–12 weeks of protected range of motion. Active strengthening begins at approximately 3 months. Full return to overhead activity or throwing sports typically occurs at 6 months, with some high-demand athletes taking up to 9–12 months.
Total Shoulder Replacement
Most patients achieve significant pain relief within 6–8 weeks. Full functional recovery, including return to recreational activities, typically occurs between 3 and 6 months. Strength and endurance continue to improve for up to 12–18 months post-operatively.
Reverse Shoulder Replacement
Functional gains often occur faster than with anatomic replacement, as the reverse design compensates for deficient rotator cuff function. Many patients experience meaningful pain relief within 4–6 weeks. Full recovery follows a similar 3–6 month trajectory.
When to Get a Second Opinion Before Surgery
A second opinion is not a sign of distrust — it is a standard part of responsible surgical decision-making, and every qualified surgeon will tell you that. Specifically, consider seeking one when:
- You’ve been recommended surgery without a trial of structured physical therapy
- Your surgeon cannot give you a specific complication rate for your planned procedure
- You have multiple health conditions that increase surgical risk
- You’re being told there is no non-surgical option, but haven’t seen a sports medicine physician
- You feel rushed or that your questions weren’t fully answered
FSI actively welcomes second-opinion consultations. Dr. Varma provides an independent assessment of your imaging, diagnosis, and proposed surgical plan — without pressure toward any particular course of action.

Get a Clear Answer Before You Decide on Surgery
Dr. Varma and the FSI team offer comprehensive shoulder evaluations — including imaging review, diagnosis, and a frank discussion of your surgical and non-surgical options. No pressure. No runaround.
Call or text: (352) 404-8956 · 1925 Don Wickham Drive, Clermont, FL 34711 · Walk-ins welcome
Frequently Asked Questions
Medical Sources & Authority References
- American Academy of Orthopaedic Surgeons (AAOS) — Shoulder Surgery Overview
- NIH / NCBI — Nerve Injury in Shoulder Arthroplasty: Systematic Review
- Mayo Clinic — Shoulder Surgery: Indications and Risks
- Harvard Health Publishing — Shoulder Pain: Diagnosis and Treatment
- CDC — Cutibacterium acnes (C. acnes) Surgical Site Infections
Related Articles from Florida Sports Injury & Orthopedic Institute
- Complete Guide to Shoulder Surgery at FSI — Types, Candidates, and Outcomes (Money Page)
- Rotator Cuff Repair: Surgery vs. Conservative Treatment — What the Evidence Shows
- Physical Therapy After Shoulder Surgery: Why Your Protocol Matters More Than the Operation
- PRP Therapy for Shoulder Injuries: What It Is and When It Works
What FSI Patients Say
Dr. Varma walked me through every possible risk before my rotator cuff repair. Nothing surprised me in recovery because he prepared me for all of it. I was back on the tennis court at six months — exactly when he said I would be.”
Medical Disclaimer: The content on this page is provided for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Individual results vary. Always consult a qualified physician or licensed healthcare provider regarding any medical condition, symptoms, or treatment options. Do not disregard or delay seeking professional medical advice based on information read on this page. Florida Sports Injury & Orthopedic Institute · 1925 Don Wickham Drive, Clermont, FL 34711 · (352) 404-8956.









Leave a reply